|
My mom was diagnosed with Lupus back when I was in middle school. Looking back, it all made sense. Every time we went outside when I was a child everyone would always comment on how red she was. She wasn’t sunburnt, she was just red. It mainly affects her face (hint: Lupus butterfly rash) but it will also affect her chest and upper arms. She also had quite a few hip problems, and no one could really figure out what was going on. She was finally referred to a rheumatologist after some funky lab work. She was soon diagnosed with Systemic lupus erythematosus (SLE). Her lupus mainly affects her joints and some doctors believe she also has RA.
Flash forward a couple years and I began having problems with occipital neuralgia and chronic migraines. The first neurologist I saw did some thorough lab work to see if there was something causing it that we didn’t know about. When we got the results,my antinuclear antibodies were elevated, and I had a homogeneous pattern. They wanted me to go see a rheumatologist and so I went and saw the same on as her. My very first appointment he wanted to diagnose me with arthritis, but I refused to accept the diagnosis and blamed it on gymnastics (I was a gymnast for 14 years prior). Three years later and in college and I started seeing a new rheumatologist in my college town and finally accepted my initial diagnosis of inflammatory arthritis. She did not diagnose me with Lupus but she went ahead and started me on Plaquenil to slow the progression because between my lab work and my mom’sdiagnosis there was no doubt I would shortly be following her path and we wanted to slow it down as much as we could. Since then I began getting the butterfly rash which we weren’t sure if it was related to my Trigeminal Neuralgia or Lupus. I didn’t agree with several things that she wanted to do so I switched doctors and am now seeing one at UTSW where I was officially diagnosed with SLE and Nonspecific immunological findings in addition to the arthritis. While I wouldn’t wish this diagnosis on anyone, I am glad I am going through it with my mom. She is ahead of me in the progression of the disease, so I know what the future holds for me. This help me mentally prepare for the future and cope with it. We have both been on several medications so we can compare our experiences and together we figure out what will be best for each of us. Wouldn’t want to go through this with anyone else! Name?
Savanna Braun Age? 23 Type of RA and lupus? Polyarticular Psoriatic Arthritis with Spondylitis and Enthesitis, was JIA since the obvious onset was around age 13/14 How does it affect your daily life? My daily life consists of going to classes, studying, completing assignments, doing something with at least one of the clubs I’m in, and, of course, being with friends. This disease, along with some other ones, are woven through this and have really been a deciding factor in just about everything. I go to school in the place I do now because it has a small campus that I can get around, an issue I learned of when I went to a huge campus my freshman year, and that the air quality is decent, along with the fact that there are trees everywhere, which makes me happier. The schedule of my classes and amount of courses I take are planned out to give me the ability to nap a lot during the day, which I need to do, while still allowing me to have enough time to study & do my work for. The clubs I’m in are not at all physically demanding, most of the official things to do are very low activity if anything, this works for me because my body would not be impressed with me joining a rock climbing club, which I’d love to do but cannot. Even down to the friendships I have, if they are highly active, adventurous people, we aren’t going to be hanging out a lot. My closest friends at school all like to just hang out at each other’s places, watching something, talking, all things I’m usually perfectly okay doing, they are even happy to tag along on my medical errands, which is wonderful because I’ve always felt they interfered with my ability to be with people for as long as we want. And of course, my being able to do all of my treatments can change my plans, like if I have my fistful of pills to take at their scheduled times or can I get back home to do a nebulizer treatment since it’s not portable. Biggest of all, it can make me unable to do anything I need and/or want to do because I’ll be in too much pain or fatigued or have been doing too much and know I have to slow down. Do you have triggers? My biggest triggers for feeling miserable or flares are doing too much and continuing to say yes to things, not sleeping enough, stress, infections, staying still too long, even weather changes, like with rain or extreme temperatures (anything outside of 60-80F). What do you want people to know? The biggest thing I’d like people to keep in mind is the variability of these types of conditions, I can be living in a way that’s pretty normal, and then it will blow up. I’m often not going to have obvious physical manifestations, regardless of how bad I’m feeling, and that can be confusing for people. This is in no way a suggestion to examine me closely, but sometimes the less obvious predictors of how bad I’m feeling are how dark circles under my eyes, makeup, walking pace, paleness, skin mottling, breathing, how talkative & loud I am, speed of talking, focus level, eating, etc. Name?
Kallie Middleton Age? 19 What food allergies do you have? Peanuts and tree nuts When were you first diagnosed? 12 How does it affect your daily life? I have to read labels on everything I eat and watch what I eat. What happens when you eat something you are allergic to? My throat and tongue swell, I break out in hives, and since I have asthma it causes an asthma attack. How has it changed as you have gotten older? No change that I know of What do you want people to know? Food allergies are nothing to play around with, they are very serious and potentially life threatening. Also, do not make someone that has food allergies feel bad or make fun of them for it.   My journey with the feeding tube started July of 2015, a little less than a month after I was diagnosed with Gastropareisis. Gastropareisis is a digestive issue that basically means partial paralysis of the stomach. This means that when someone with eats a meal or drinks a beverage, the contents can sit in the stomach for hours, or even days. Symptoms ranged from mildly annoying to so severe that some people can't even eat or take in fluids, so they have to rely on feeding tube or TPN to survive. What causes it is unknown, but it is believed to be caused by a damaged vegus nerve. I was diagnosed with it in June of 2015. I didn't get the feeding tube right away. At first we tried Reglan to help move things along, but that really wasn't helping. I also have been pumped so full of Zofran, that it's not really effective anymore. Then we tried other options such as Erythromycin, and then we tried Botox injections. My weight kept dropping. The doctor in the hospital told me that we were going to do a feeding tube next, the dreaded NJ (nasal gastric tube). She popped in my nose, and down it went. It was so uncomfortable. I was finally discharged, and then I kept tube feeding about a month, until I saw my GI. After that, I tried making some adjustments to my diet. That helped some, but I still wasn't getting proper nutrition, and I kept puking my NJ tube out, so then I found myself admitted again. The doctor told me that we were going to try a GJ (gastro jujenostomy) tube next. It was easier to hide than a NJ tube. Putting that in was so uncomfortable. The doctor had to put a tube down my nose and pump air into my stomach, then he gave me a local anesthetic, and punctured my stomach to place it. I spent the night at the hospital. I've had it for about 3 1/12 years. I don't really feed much anymore, as I still try to get my intake orally. My weight has been stable, but my gastroenterologist and my primary want me to use it because they said if I needed major surgery for my other issues, that I couldn't get it since my weight isn't right. Something I struggled with is that I'm really self conscious about my body. Before I was chronically ill, I was physically fit, but unfortunately my health started to decline, and I lost all that muscle and weight. I'd love to put it on through working out, instead of the tube, even though my doctor wants me to continue feeds. I still use it for draining and meds though.
*I think you should stay: I promise it gets easier once you decide to get help- I promise you can heal from the darkness.*
There once was a girl whose life fell apart over and over and over until one day on her 19th Birthday she decided she really couldn't take the pain of all the endings so she got a bunch of pills, her favorite drink to swallow them with and her pillow and teddy bear and went to be alone and die. On the way to the location she had decided on she passed her Mom in her car and took it as a sign that her Mom didn't notice her so she kept on with her plan and tried to kill herself on her very own Birthday. That girl was me. There were lots of reasons why this happened but basically I was trying to kill the pain in both my body but especially my mind: my physical pain tortured my mind. I texted a friend to say goodbye as I drifted off to what I hoped was forever sleep and my friend ended up finding me and getting me help. I remember the EMTs making me drink charcoal in the ambulance and I kept spitting it out. When we got to the hospital I realized how badly I had wounded my family. I remember my sister who I always had a difficult relationship with came to the hospital and I was pretty surprised that she was there. Despite realizing that I hurt my friends and family my pain was a lot deeper than my desire not to hurt the people I loved: I actually ended up attempting suicide at least 5 other times over the next 8 years (I don't care to count how many times I attempted because it's really sad to me) My mental health was really up and down for awhile and then it got really bad until I was eventually diagnosed with Borderline Personality Disorder. I think the worst part of BPD was how I'd be happy and one tiny thing would flip my mood and make me decide I wanted to die. All of these symptoms were heartbreaking for my family and really embarrassing to me: so embarrassing that I didn't want to own my mental illnesses which prevented me from healing. If you can't admit you have a mental health problem it's not really possible to get better from it. I was hesitant to admit I was mentally unstable because there is a ton of stigma surrounded by mental illness, especially BPD. The #1 thing people with borderline are called is narcissistic and if you get to know me you know that although I'm overly sensitive I'm extremely kind and thoughtful. Eventually I decided to go to a DBSA*** meeting (Depression Bipolar Support Alliance) because my Mom was going to the meeting for friends/ family members of people who have mental illnesses. She went for 2 years before I finally caved and went to the patient meeting: I was mortified that she went to these meetings because of ME. But DBSA was what turned everything around for me because I finally admitted I was not ok and that I wanted to get better. For years before I did DBT*, COG** and private therapy but they didn't really help because I didn't really want the help. I'm happy to say that I don't have any Borderline symptoms at all anymore except that I'm pretty sensitive and I haven't attempted suicide or been inpatient psych since 2015. I also don't require regular therapy anymore but I still keep up with my Psychiatrist and am on an antidepressant and a sleeping medication. If you are struggling please don't hesitate to reach out and if you know someone who is mentally struggling please don't judge them but lovingly guide them to resources. I believe by sharing our stories we can end the stigma associated with mental illnesses so in the future people struggling won't be afraid to get therapy or go to a support group. 💕Rest in peace Anthony Bourdain and Kate Spade 💕 *DBT or Dialectical Behavior Therapy is a set of skills that center around mindfulness, emotion regulation and distress tolerance: this therapy is especially beneficial for people with Borderline Personality Disorder. **COG or Cognitive Behavioral Therapy is a treatment method designed to shift faulty thoughts and behaviors to healthier ways to deal with problems and stress. *** DBSA stands for Depression Bipolar Support Alliance: it is a support group made for both patients as well as friends and family members of people impacted by mental health issues. To see if there are meetings in your city simply Google "DBSA" along with the name of your city or region. - Written by Sarah Wheeler Trigeminal Neuralgia is a thief. Out of all of the diseases I battle, Trigeminal Neuralgia is the biggest jerk I've ever met because it makes it hard to smile and has forever changed my dimpley, sweet smile.
Beneath the surface: My face is stiff from Botox treatments, swollen from steroids and it's just not what it used to be because TN sucks. 3 years ago I had a radiation surgery that "fried" my Trigeminal Nerve and I'm pretty sure that also altered my appearance. It feels different to smile... forced, uncomfortable and unnatural. Sometimes people don't recognize me and it's embarrassing. Sometimes people make comments like "Your so much prettier when you smile" and it hurts. Although the treatments for this disease have changed my appearance I'm super thankful because on most days I'm in a lot less pain. But tonight things are very bad and I don't feel like myself: in fact I feel pretty "Dark and twisty". You see I've been trying to kick this pain in the left side of my face for the past 6 hours. I'm exhausted but it feels like my face and jaw are being electrocuted so I'm wide awake. I've tried multiple medications including muscle relaxers, anti inflammatories and opiates. I've tried essential oils, pain salves, CBD, ice, heat and the list goes on. I've tried to distract myself with art projects, making care packages for others, watching movies, etc and nothing has helped... its 3 am and I'm starting to panic. What if I can't sleep at all? What if the pain gets worse and I need to go to the ER? Who will take me? Will the Dr be compassionate or asshole? Currently I can barely open my jaw, I'm unable to brush my teeth, eat/ drink and I'm insanely nauseous from the pain. I'm tired. I want to sleep. My face hurts. I cannot cry because that will make it worse but I'm starting to panic... This is a lot for anyone to stress about at 3 am and although it's not "fun" it's become my job because I'm 30 and stuck on permanent disability. I just really miss my cute face. I might not smile the same as I did at 16 but these disease has made me resilient and for that I'm thankful. Written by Sarah Wheeler April 24th, 2018 By Jennifer January 28th is SMAS Awareness Day. SMAS, or Superior Mesenteric Artery Syndrome, is a vascular disorder with digestive consequences. When the space between the Superior Mesenteric Artery and the aorta is too small for the duodenum (the beginning of the small intestine), to pass food through, it can cause extreme pain and intestinal blockage resulting in possible hospitalization and can lead to sepsis and even death. SMAS is really rare. There are statistics that say there are as few as 500 to possibly as many as 10,000 people in the U.S. who suffer from this disease. However controversial the diagnosis, I had a surgeon put it in these simple terms: SMAS is a disorder of plain geometry. A normal person has an angle between the two arteries of 38-56 degrees and at least 10-12mm of space for food to pass through the duodenum. With SMAS, the Mesenteric fat that pads this space and holds it open is missing, which collapses the two arteries and the resulting angle and space is too small to allow food to pass through. For instance, my angle is 11 degrees and width is 7mm, considerably smaller than normal. This can cause extreme pain and nausea for hours, even days, after eating because the food has nowhere to go. Aloha, I’m Jennifer from Hawaii, and I’ve been suffering with SMAS since 2013. My abdominal pain would get so bad and last so long I’d have to go to the emergency room at least once a month, sometimes once a week. I lost 70 pounds in nine months. I had many tests done like a colonoscopy and endoscopy, a mini pill camera, and other scopes and scans to try to diagnose my extreme pain. However, because the cause of my blockages was coming from the outside of my intestines, not from inside where everything was scoped, doctors couldn't see anything wrong. Therefore, like many SMAS patients, I went through a very stressful period where I was misdiagnosed and not believed. Because of weight loss, malnourishment, and inability to eat due to pain, I was misunderstood and misdiagnosed at first as having an eating disorder. All my pain and emergency room visits were blamed on my supposed inability to handle stress. At doctors’ suggestions, I spent more time in therapy trying to figure out if there was a mental reason why I was in pain and couldn’t eat, than I spent in doctor’s offices seeking a medical origin and solution. I knew within myself that my problem had a medical origin, but couldn’t get anyone to listen to me. I went through a few doctors before I found one caring enough to try and research my symptoms. Recently, I read a medical article about SMAS in which the doctor likened SMAS-related pain to that of late-stage pancreatic cancer. Even though it’s difficult to compare pain, I felt vindicated to know that my pain is real and in reality, that it is severe. I’m not a wimp, it’s not in my head, I’m not causing it directly or indirectly, and there’s nothing I can do about it. I am not a drug-seeker. Finally, in an ER visit, the problem was seen on CT scan and recognized by a gastroenterologist, and I had caught my SMAS on camera and was correctly diagnosed. I had corrective surgery for my SMAS this last spring. SMAS is a difficult disease to overcome; out of all SMAS patients who have had corrective surgery, only 1/3 see improvement of symptoms, 1/3 see no improvement, and 1/3 have worsening symptoms. Since I joined an SMAS Support Facebook group almost a year ago, two members have passed away from this disease. I have been so sick that I am unable to work and, at times, even care for myself. My best hope for remission of symptoms is to gain enough weight to replenish my missing Mesenteric fat pad that holds the arteries open around my small intestine. My life had been turned upside down as a result of SMAS. The most surprising lessons I’ve learned is how difficult it is to get medical professionals to take you seriously when your symptoms are not easily explainable, and how helpless and horrible it feels to be medically mistreated. As a result of the trauma I’ve endured as the hands of doctors who, for instance, blew me off as being a “drug seeker” when I had a severe intestinal infection that required immediate antibiotics, or insisted I had an eating disorder because I couldn’t keep food down, I vow to be a vocal and powerful medical advocate for myself and anyone else who needs help being heard. The silver lining is, of course, that I am incredibly thankful for all the big and small things. I developed a deep meditation practice through the process of being sick, and my level of compassion for others and desire to help has naturally grown. I have learned to find deep fulfillment and happiness despite being slower, dependent, and limited. SMAS is a devastatingly difficult and misunderstood disease. Like with any and all illness, we who suffer from SMAS have no choice but to rise to the occasion. We are survivors and warriors. By Ron
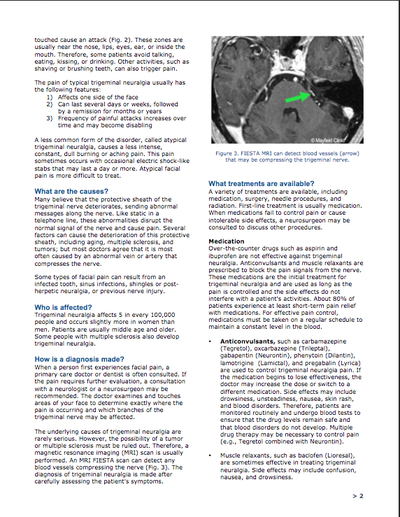
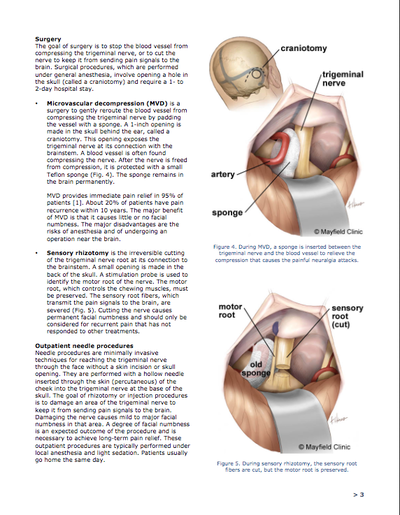
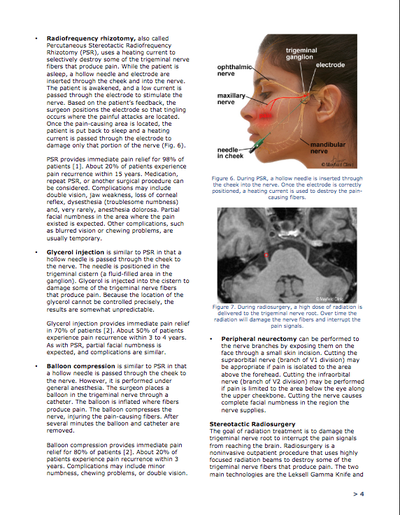
One of the hardest parts of being chronically ill, for me, has been having to change my career plans. Finding fulfillment and a purpose in life, for me, has always been tied to helping other people. Being chronically ill made it necessary to reevaluate my future and replan what is going to be best for my health. I Can't help others if i'm not in a good place myself. This is a part of spoonie life I haven't seen discussed a lot, so I thought I would share my story. For all of my life, I had always planned on a career as a medical provider. Originally, my plan was to go into neurological surgery, but after having five neuro procedures myself, it would no longer be safe to operate. I switched from a premed track into a medical physics track, as its less of a physical job and more of a mental one. Unfortunately, due to the operations and later the medication I have to be on to control my severe nerve pain, that became very hard. My gpa plummeted and it was suggested I do a medical withdrawal from the program. My attendance was horrible, as I was in and out of the hospital frequently and debilitated with severe pain. I had a really hard time accepting that it would no longer be safe to be a medical provider. I struggled for a few years with it, and kept searching for ways to change this. In 2016, one of the worst things to happen medically occurred, but it was one of the best things that helped me come to peace with the predicament I am in. I had a small brain stem stroke while driving. I went unconscious and was involved in a serious single car accident. Luckily I was not injured. This really put things into perspective for me, as to how serious and unpredictable my health really is. Since that time, I have had 11 transient ischemic attacks and another stroke. Add onto all of this the fact that I have been having problems with my legs, and lately have been getting around with crutches, to all of this and I am slowly coming to the realization that any job that puts me on my feet is not in the best interest of my health. I currently work part time as a pharmacy technician. It's a job that I absolutely love! But last year, one or two short shifts was all I was able to work due to pain and the weakness. I was on leave a fair amount due to surgeries, a stroke, and flare ups. It's not the way I would like things to be and right now, I have been on leave since around the first of the year. I am coming to terms with the fact that I may not be able to work much longer, let alone work in the field I had been dreaming of since I was a child. I'm having more tests soon, and will be talking to my doctor about possibly starting the process to file for disability. It's a topic we've talked about on and off for a year or so, trying to get me to be more receptive of the idea. It's a very personal decision. My PCP (who I have an amazing relationship with) said that i'll know when its time. Well, I really feel like it is. My biggest worry was that if I stopped working, I would not feel fulfilled in life. I have always been someone that got joy and fulfillment from helping others. Not working in healthcare, how would find happiness and purpose in life? Well, I have found purpose and fulfillment by getting involved in the chronic illness community, helping other people coping with chronic conditions how to live the best life possible. I have also found a niche talking to students studying healthcare occupations and introducing them to the other side of the equation. Hopefully by doing that, I can help the next generation of doctors, nurses, etc learn how to help those of us who are sick better. For those of us who are “type A” personalities and always like to have an ironclad plan, changing those plans and reworking them is a challenge. I have always been a planner. I had my whole life planned out, all the way down to which fellowships I wanted to do. Slowly, I am learning to relax a bit and go with the flow. This has been a huge improvement for my mental health. I am learning that there are other ways to find purpose and fulfillment in life, other than just work. I wish I would've learned this sooner. But I guess, better late than never! Trigeminal Neuralgia is known to be one of the worst pains known to modern medicine. It causes sharp electric like shocks that travel through the face. It is also incurable. Medications, surgery, and alternative therapies can help put the pain into a remission or make it more tolerable, but it's a life long condition. And it's a condition that a lot of people are not familiar with, and many of us in the Trigeminal Neuralgia community are trying to change this. What follows is the "readers digest" version of my story with this condition. -Ron My story is not like most. I am 24 and have Trigeminal Neuralgia. The pain started in late March of 2013. It was not all the time, but very debilitating when it struck. I lived with this until early summer, when the attacks became more frequent, went to my primary doctor who thought that I had some knots in my muscles on the left side of my face. I was prescribed muscle relaxers. They did nothing. His next thought was TMJ. I tried the NSAID medications and saw my dentist (as my primary doctor asked me to). My dentist said definitely that what I have going on is NOT anything he can treat and to go back to my primary doc. When I went back with this information, I saw him and his partner, who also did a full evaluation. They both agreed that the symptoms I have are caused by Trigeminal Neuralgia. That was in October of 2013. Prior to that in August, I left my retail job and did so at just the right time, pain had increased to the point that I could hardly function. That led to the diagnosis. November was a very hard month, I was unable to drive due to the pain and the pain medications they had me on until I could get a pain management consult. That happened in December. He immediately put me on Gabapentin. What a nightmare the time to follow was. I had severe memory loss. I could not remember the day, date, where I put stuff, and worst of all, I could not ever remember how I wanted to finish my own sentences. I went back and told my doctor that this medication is a nightmare and I felt like I was going into early onset dementia. This freaked him out, and he told me to go off the gabapentin cold turkey (not recommended, but necessary). I started Lyrica the same day. The pain improved significantly and my memory started to return. By late January, I was back to normal (after the gabapentin and a bout of pneumonia). I had an MRI in late January. It came back clean. The pain hit a high in February, and I had to wait till mid-march to see a neurologist, so I decided to try Upper Cervical Chiropractic care. The neurologist had nothing to offer, except for Tegretol, which I allergic to. I did not see her again. I continued to see the chiropractor until mid April, when the adjustments started to hurt. During this time, I began seeing another interventional pain specialist who began doing a type of nerve block called the SphenoCath. These are non invasive SPG blocks. The first one I had in April 2014, and the second in May 2014. They did work. I began having pain during the Upper Cervical adjustments, and my pain doctor told me to stop seeing the chiropractor and to get an MRI. The MRI showed a few disc herniations in the cervical region. PT was started immediately and so was TENS therapy. At this time, I was being evaluated for a genetic condition that runs in my family, Acute Intermittent Porphyria (AIP), due to some issues I was having with the medications. In June, 2014 the diagnosis was positive and the pain specialist told me she could no longer treat me due to the risks. Back to square one. I sought out a neurosurgeon and found an amazing one here in St. Louis. He suggested MVD surgery, but I was not ready at that point. MY PCP handled the medications while we searched for a neurologist to handle my case. I got lucky in August, 2014 when I found a great neurologist who understood TN. She also confirmed the diagnosis and we started down the list of medications. I began taking Vimpat. This helped a bit, but due to side effects, we couldn’t dose it higher, so Trileptal was added. I started college during this time too. At the start, all was well. I was having no issues, the medications were helping, and all was well. Then October came, and I ended up in the ER with a major flare. This was a wake up call that something had to be done, so I called the surgeon and asked to schedule an MVD. It was scheduled for December 17th and I made an appointment with him in November to have some questions answered. My attendance at school became spotty at best. Luckily I was covered by disability services and a plan was worked out. I ended up in the ER again in November with major pain. At this point, I was only on Trileptal due to cognitive issues, which were impairing my ability to function at school. I made it to my surgery date as soon as I could. But as with any nerve pain, the Trigeminal Neuralgia had a mind of it's own. All in all, from December 2014-October 2015, these are the operations I had: 12/2014: Left side MicroVascular Decompression 1/2015: Left Balloon Compression Rhizotomy 5/2015: Left Side Partial Sensory Rhizotomy 6?2015 Left side wash-out craniectomy for infection 10/2015: Right side Microvascular Decompression and Partial Sensory Rhizotomy Having five brain surgeries in one year is very hard on the body. Unfortunately due to this, I had to withdraw from university for medical reasons. It took me about a year to fully recover from all this. After about a year, the TN pain became more manageable. Today, I am doing magnesium infusions every three weeks, sphenopalatine ganglion nerve blocks as needed, and still taking the anti epileptic medications. The pain is much more controlled that it ever has been, and while I still need pain medications, I am able to live a much more quality life. The Following are images of the Trigeminal Neuralgia information found on the Mayfield Clinic website. This is among the best and most concise information i've found for this condition.
t’s a 4 AM wake up call that’s not going to stop.
|
Categories
All
|




 RSS Feed
RSS Feed
